WRIST FRACTURES
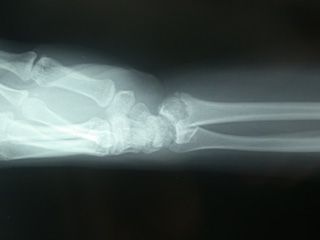
The wrist is a structure consisting of 8 small bones and the articulation of two bones in the anterior arm. The wrist bones are connected by tight ligaments. This structure allows the wrist to move freely in all directions. Wrist fractures usually occur after falling on the hand when the arm is open. Fractures may occur due to high-energy traumas such as traffic accidents or falling from heights. Osteoporosis in the elderly causes the bones to become thinner and become more fragile. Wrist fracture may occur with simpler traumas in elderly osteoporotic patients. The most fractured bone of the wrist is the forearm bone called radius. When fracture occurs, wrist pain, swelling and deformity are observed. (Figure 1)
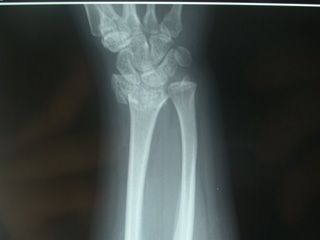
Sometimes the fracture may not dislocated or bone ends can be conmpletely separated from each other. Also the fracture can be very fragmented and completely displaced. Treatment varies according to fracture type. The first thing to do is to put the wrist over a stable object (cardboard, board, etc.) and prevent it moving more. A fracture is detected after radiological examination. A CT (computerized tomography) examination is performed. Detection of the fracture parts can be observed by CT examination as 3D. Fractures of the joint surface are important for the evaluation of future treatment and further result. Sense and movement examination should be done with a level that the pain allows. If some of the fractures are out of the skin (open fractures), it has a more risk of infection. Even if fracture treatment is completed, patients with this type of fracture should be hospitalized for a certain amourt of time and should be given antibiotic treatment. During the decision of treatment, the patient's age, activity level, jop, hobbies, whether he has had a previous wrist trauma, or other medical problems should be evaluated.
In radiological examination, the fracture extention to the bone, fragmentation the fractures slipperiness and the fractures stability should be evaluated. All of these factors should be brought together and the most appropriate treatment decision should be taken for the patient.
If the fracture sides are not displaced, it is sufficient to fix the fracture with plaster. Fracture fixation period (between 3-5 weeks) is determined according to the age and fracture type of the patient. If fracture has been dislocated, after the evaluation of the fracture, it is tried to put into place. If it is possible, the fracture can be seen with the help of a radiographic examination (scopy) which can be performed instantly. If the fracture is in the proper position, plaster can be made. If there is no scopy, after being taken to the plaster, radiological examination is performed and the fracture position is evaluated by taking the again. If it is decided to continue with plaster, radiological examination should be done 3 weeks later and whether the fracture position is dislocated should be followed. Plaster is removed 5-6 weeks after.
If the fracture is considered as multiple, intra-articular and unstable fracture, surgical treatment decision is taken by considering the general condition of the patient.
In surgical treatment,
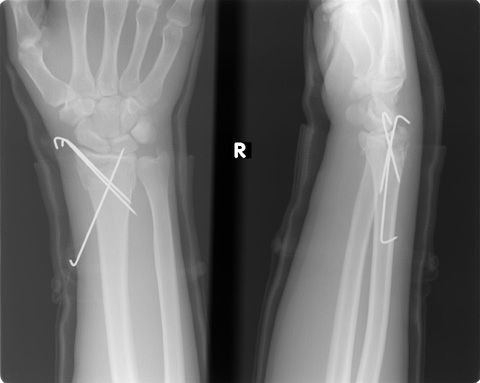
• After fracture correction, fixation with pins from outside under the control of the scopy and plaster.
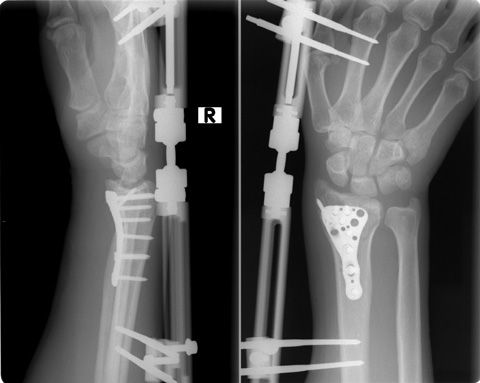
• Detected by externally placed materials on both sides of the broken pin (external fixator)
• Correction of broken parts by open surgery, can be detected with the help of plaques and screws after.
Arthroscopy can be used to evaluate the joint surface in some cases that intraarticular fracture is detected. Particularly in patients with bone resorption and in multi-part fractures/fracture stabilization is increased by placing bone fragments (bone grafts) taken from other parts of the body and helps accelerate the union.
The plaster is removed after the bone setting. There is a possibility of movement limitation after removal of plaster. Physiotherapy is very useful during this period. This varies due to personal factors. While using the wrist, pain and swelling occur for a time.








